Похожие презентации:
Nonrheumatic carditis in children
1. Nonrheumatic carditis in children
2. Plan of the lecture
1. Definition of carditis
2. Etiologic factors
3. Classification
4. Clinical presentation of carditis
5. Treatment
6. The differential diagnosis of
cardiomyopathy
3. Nonrheumatic carditis (NC)
• NC join all inflammatory myocardium diseasesof different etiology that aren’t caused by bhemolytic Streptococcus of group A and diffuse
connective tissue diseases
• NC is polyetiologic disease
4. Epidemiology
• According to autopsy data morbidity in childrenhigher than in adults and is 9,4%.
• Severe forms are more frequent in children
especially in infants.
• In children died from sudden death mortality
due to NC is 17 %.
• NC morbidity increased during viral disease
epidemia.
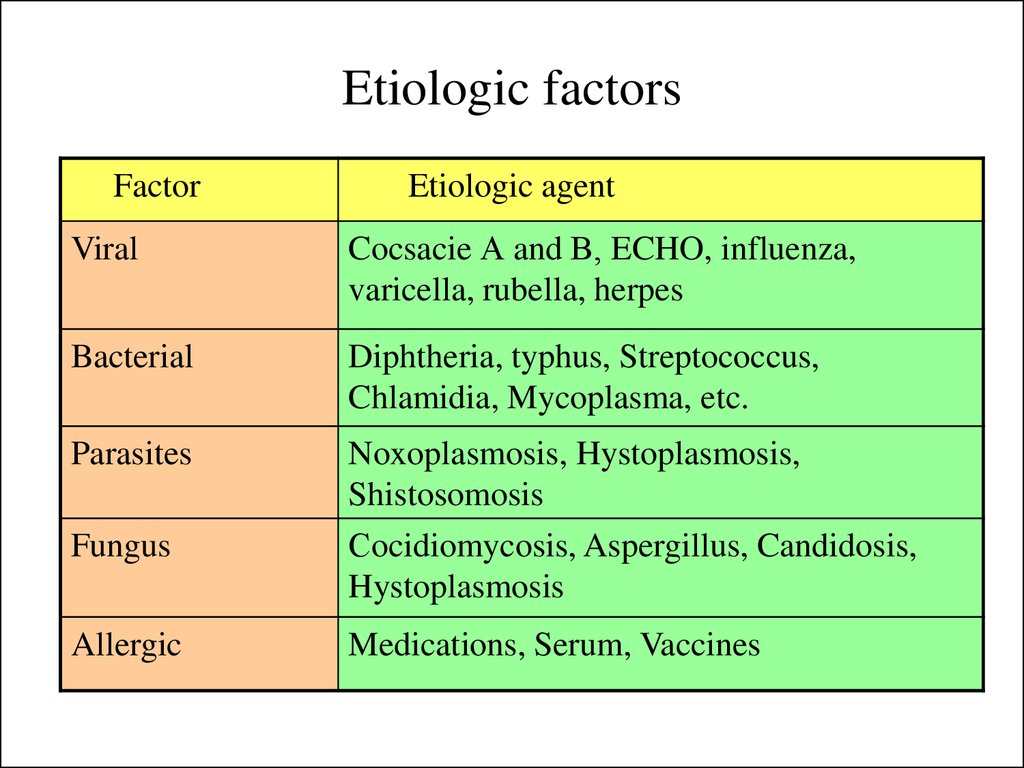
5. Etiologic factors
FactorEtiologic agent
Viral
Cocsacie А and В, ECHO, influenza,
varicella, rubella, herpes
Bacterial
Diphtheria, typhus, Streptococcus,
Chlamidia, Mycoplasma, etc.
Parasites
Noxoplasmosis, Hystoplasmosis,
Shistosomosis
Сocidiomycosis, Aspergillus, Candidosis,
Hystoplasmosis
Fungus
Allergic
Medications, Serum, Vaccines
6. Predisposed factors
• Inherited myocardium hypersensitivity• Inherited immune deficiency
• Vasculitis
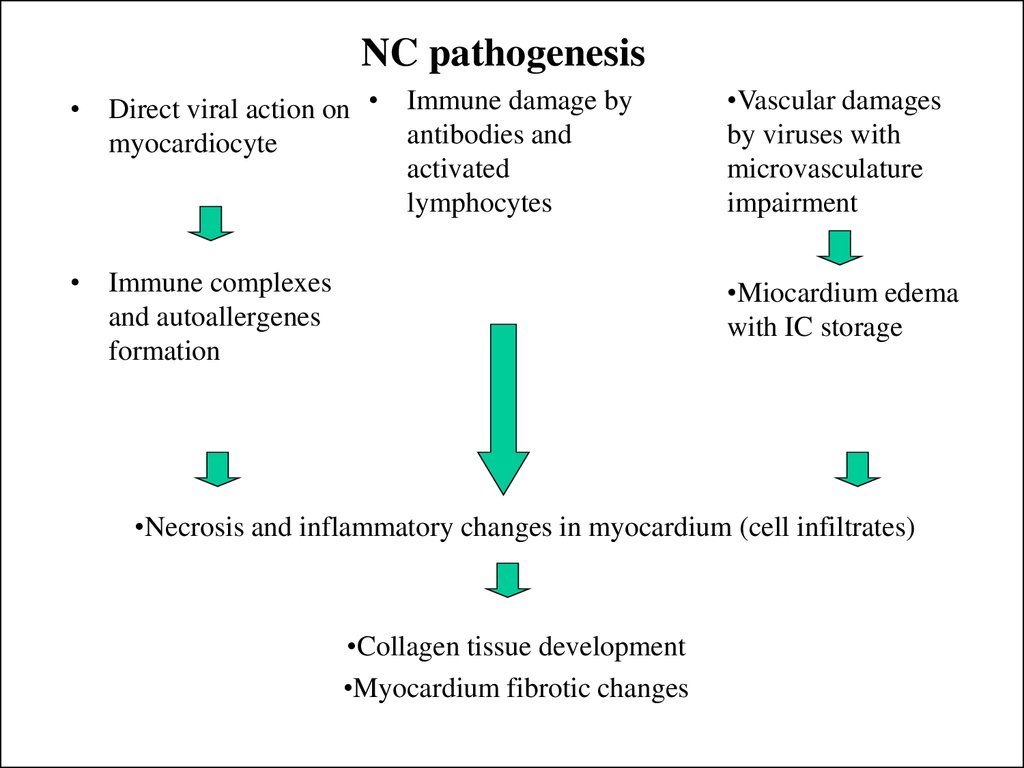
7. NC pathogenesis
• Direct viral action on • Immune damage byantibodies and
myocardiocyte
activated
lymphocytes
•Vascular damages
by viruses with
microvasculature
impairment
• Immune complexes
and autoallergenes
formation
•Miocardium edema
with IC storage
•Necrosis and inflammatory changes in myocardium (cell infiltrates)
•Collagen tissue development
•Myocardium fibrotic changes
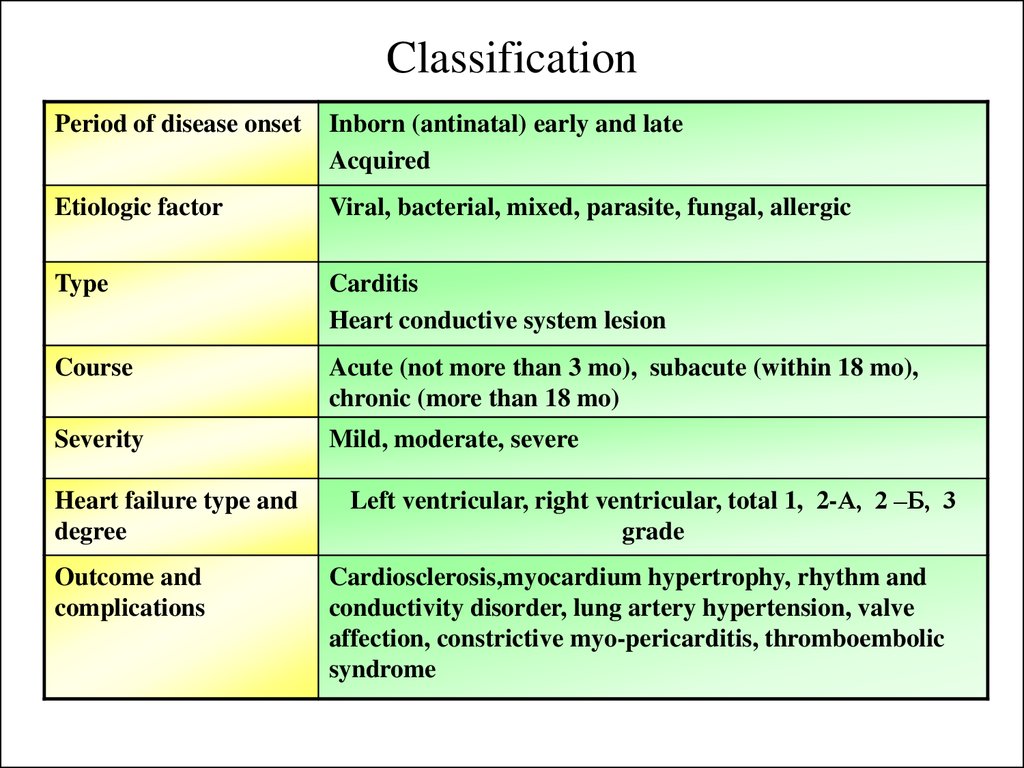
8. Classification
Period of disease onsetInborn (antinatal) early and late
Acquired
Etiologic factor
Viral, bacterial, mixed, parasite, fungal, allergic
Type
Carditis
Heart conductive system lesion
Course
Acute (not more than 3 mo), subacute (within 18 mo),
chronic (more than 18 mo)
Severity
Mild, moderate, severe
Heart failure type and
degree
Outcome and
complications
Left ventricular, right ventricular, total 1, 2-А, 2 –Б, 3
grade
Cardiosclerosis,myocardium hypertrophy, rhythm and
conductivity disorder, lung artery hypertension, valve
affection, constrictive myo-pericarditis, thromboembolic
syndrome
9. Inborn carditis ( are rare,especially isolated ones)
Early(causative factor affects within
4-7 mo of gestation;
inflammatory reactions are
absent but tissue prolifiration
is present)
• Fibroelastosis
• Elastofibrosis
Late
(appear withing last 3 mo of
gestation; inflammatory
reaction is developed)
• Fibrosis is absent
10. Clinical picture of early carditis
• Neonate usually has signs of carditis withcontractile dysfunction and heart dilation
• Main symptom is cardiomegaly and congestive
heart disease, dyspnea, cough
• Sometimes congestive heart disease manifest itself
after viral diseases
• Body weight gaining retardation, paleness,
flaccidity, sweat, naso-labial cyanosis, weak
suckling
11.
Clinical presentation of late carditis• Manifest at 1-6 mo old,sometimes later at 2-3 years old.
• Neonates has normal body weight but than retard weight
and height gaining due to progressed congestive heart
disease.
• Children have frequent common cold and respiratory
diseases
• Skin is pale with perioral cyanosis.
• Flaccidity, weakness especially during feeding, attacks of
agitation, convulsions, acrocyanosis
• Constant tachycardia, dyspnea during rest and crying.
• Stable rhythm and conductivity disturbances
12. Objective data of inborn carditis
• Heart borders are dilated to left and up, apex beatis wide, early formation of “cor hibus” that is quite
visible at 5-6 mo old.
• Auscultation : muffled 1 sound at apex ans
accentuated II sound at lung artery. If congestive
heart disease progresses gallop rhythm appear.
Systolic murmur can appear due to relative mitral
valve insufficiancy.
• Congestive heart disease in fibroelastosis is –
resistant to treatment that differ it from acute or
subacute carditis.
13. Additional examining methods
• ECG: Sinus brady- or tachycardia, conductivityabnormality, decreasing of waves voltage, interval Q-T
elongation,T wave inversion, deviation of axe
• X-Ray: lung pattern amplification due to vein
congestion. Heart size is increased. Shape of heart is
round or trapeziform with smoothed waist especially
for inborn carditis.
• Echo CG: endocardium consolidation, left ventricular
and atrium dilation, hypokinesia of ventricular septum,
dislocation of mitral wave to posterior wall, decreasing
of ejection fraction (less than 60% for infants and 55%
for adolescents)
• in 40 % of patients there are thrombi in apex of LV.
14. Severity of carditis is dependent of
1. Myocardium “injury” hypertrophy confirmed by ECG andEchoCG
2. Cardiosclerosis, including endocardium thickening (Echo
CG signs –contractile capacity decreasing, constant ECG
changes like intraventricular and AV- blockages,
extrasystols)
3. Pulmonary hypertension that indicative for severity and
poor prognosis : crimson discoloration of face,
acrocyanosis, II sound accentuation in lung artery, right
ventricular hypertension
4. Insuficiency of AV-valves (comparative or organic)
5. Constrictive pericarditis
6. Thrombus-embolic syndrome( neurologic symptoms –
convulsions, paresis, abdominal pains, urine tests changes,
hypertension)
15. Acquired myocarditis
Connection withintercurrent infection
• Prerequisite connection with acute viral infection.
• Flaccidity, weakness, ( weak breast sucking in infants), fast exhausting
after usual loadings ( games, studying etc.)
• On the ground of ARD symptoms resolution clinical signs of cardiac
damage progress: greyish-pale skin, naso-labial cyanosis, acrocyanosis,
dyspnea with wheesing and rales
• Obsessive cough, reinforced after changing position
• In patients with thymomegaly voice become low
• In 20% attacks of cyanosis, excitability, loss of conscience, convulsions,
vomiting can occur.
• Fever recur 2-3 weeks later
• Hepatomegaly appear as a sign of heart failure
• Sometimes very intensive abdomen pains can be as an initial symptom
and children turn to surgeon
• Arrhythmias.
• Diuresis decreasing, edema.
16. Auscultatation in myocarditis
• Muffled I sound• Tachycardia
• Systolic murmur on apex
17. Diagnostic signs in carditis
• Radiology: dilation of heart borders to left, cardiothoracal index is increasing (>0,55)• Echo-CG: left ventricular dilatation, decreased
contractile myocardium capacity (<60-55%)
• ECG:
– Decreased voltage during 2-3 week of disease, than it
become high, especially QRS and then again decrease.
– Sinus tachycardia or signs of different arrhythmias.
– ST-segment and T wave changes ( repolarization
process abnormality).
• Lab data: elevated ESR and α, γ-globulins, CRP(+),
neutrophyl leucocytosis.
• Creatinephosphokinase (CPK) and
lactatedehydrogenase (LDG) ensymes level is elevated
Right ventricular biopsy is a diagnostic standard (!)
18. Treatment
1. Strict bed regimen 8 weeks and moreaccording to functional capacity of CVS.
2. Diet № 10. Restriction of water intake,
diet is enriched by potassium containing
products: raisin, dried apricots, nuts, dried
plums etc. Medication corrector of Mg
and K drugs are asparcam, magnerot,
panangin
19. Medication treatment
• Etiologic-antibiotics ( choice of it
dependant on causative factor)
- antiviral drugs
20. Medication treatment
• Glucocorticoids -in severe coursewhen shock, heart failure are present
• Nonsteroid anti-inflammatory drugs
(NSAID)-are contraindicated in acute
phase of disease because they enhance
cell damage ( diclophenac, naproxen,
ibuprofen)
21.
3.4.
5.
6.
7.
Antibiotic treatment courses (in the case of intercurrent infection,
surgery, exacerbation of chronic infection focuses)
– Semisynthetic penicyllines: Augmentin, Amoxycilline 10-14 days
long.
– Macrolides:
• Roxytromycine – 7,5mg/ kg BID;
• Azythromycine – 10 mg/kg once per day;
– If suspicion of infective endocarditis under suspicion
parenterally: Ampicilline 100-150 mg/kg, Amicacine 2 mg/kg,
Vancomicine 10-15 mg/kg
– Treatment duration is dependent on etiology: Streptococcal -4
weeks, Staphylococcus – 6 weeks, Gr”-” bacteria – 4 weeks
Glucocorticoids in severe course (shock, allergy), congestive heart
disease, rhythm abnormalities: Prednisolon 0,8-1,5 mg/kg/day. In
viral etiology in acute phase of AVD are contraindicated as they can
enhance damage of cardiomyocytes.
Nonsteroid drugs in subacute and acute course of moderate severity
In chronic and subacute courses – aminochinoline drugs minimum
for 6 mo long.
Antiviral therapy – IV immuneglobulins in high dosages..
22. Treatment of heart failure
• Cardiotonic drugs: digoxin, strophantin, dobutamine.• Diuretics:.
–
–
–
–
Hipothiazid 1-2mg/kg/day, max – 4 mg/kg/day
Indopamide (arifon) 1,25-2,5 mg /day.
Metalazone 2,5-5 mg/day bid.
Furosemide 1-3 mg/kg/day.
• Angiotensin converting enzyme inhibitors (ACEI):
– Captopryl (capoten) 0,3-1,5 mg/kg/day
– Lisinopryl 2,5-20 mg/day
– Enalapryl (renitec, enap) 0,1-0,4 mg/kg/day
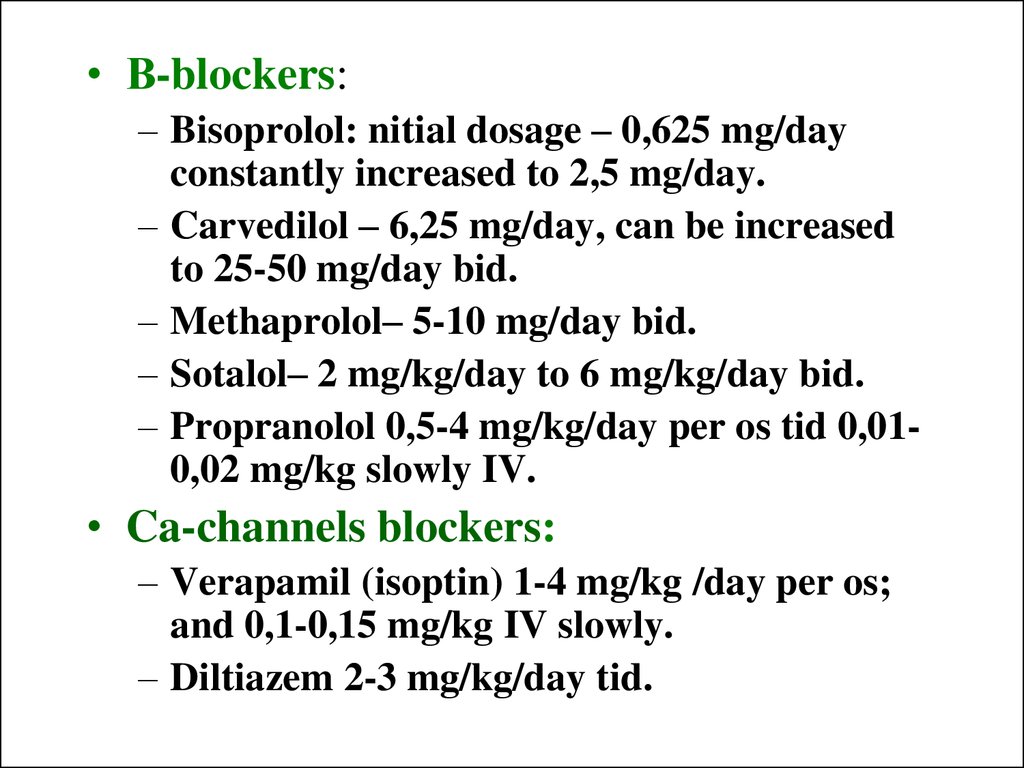
23.
• В-blockers:– Bisoprolol: nitial dosage – 0,625 mg/day
constantly increased to 2,5 mg/day.
– Carvedilol – 6,25 mg/day, can be increased
to 25-50 mg/day bid.
– Methaprolol– 5-10 mg/day bid.
– Sotalol– 2 mg/kg/day to 6 mg/kg/day bid.
– Propranolol 0,5-4 mg/kg/day per os tid 0,010,02 mg/kg slowly IV.
• Ca-channels blockers:
– Verapamil (isoptin) 1-4 mg/kg /day per os;
and 0,1-0,15 mg/kg IV slowly.
– Diltiazem 2-3 mg/kg/day tid.
24.
• Antiarrhythmic drugs:– Amiadaron (cordaron) 10-15 mg/kg/day per
os; and 5 mg/kg IV diluted in 5% glucose
– Ritmilen (dizopyramid) 5-10mg/kg/day;
adolescents 400 mg/day tid.
• Anticoagulants
- dipiridamol, varfarin
• Metabolic antiaggrigate activity
medications
• – actovegin, vitamax, vitamins (В12,
В15), carnitin,
25. Cardiomyopathies (definition)
• Cardiomyopathy (CMP) is heterogeneous groupof disease with different etiology ( frequently
inherited ones) clinically presented by
mechanical or/and electrical myocardium
dysfunction with disproportional hypertrophy
or dilatation.
• Myocardium affection can be primary or
secondary and terminate by heart failure or
sudden death
26. Cardiomyopathy
• Primary CMP-are diseases withisolated or predominant affection of
myocardium
• Secondary CMP – is myocardium
affection in systemic or polyorganic
disease
27. CMP classification
• 1. Ischemic CMP2. Nonischemic CMP: primary, secondary
2.1 Primary CMP:
2.1.1 congenital (inherited,genetic)
2.1.2. acquired
2.1.3. mixed
2.2 Secondary
2.2.1 infiltrative
2.2.2. toxic
2.2.3 storage
2.2.4 endomyocardial
2.2.5 inflammatory (granulamatous)
2.2.6 endocrine
2.2.7 heart affectionin neuro-muscular diseases
2.2.8 alimentary
2.2.9 connective tissue diseases
28. Hypertrophic CMP
• Is inherited disease characterized byasymmetric left ventricular
hypertrophy with hemodynamic
outflow obstruction and nonspecific
clinical presentation: syncope,
stenocardia, life threatening
arrhythmia
29. Hypertrophic CMP
• Obstructive with outflow pressuregradient >30 mm Hg
• Nonobstructive outflow pressure gradient
< 30 mmHg
• Latent outflow pressure gradient raises
more than 30 mm Hg only after loading
test
30.
Clinical presentation• Disease onset can be at any age.
• Disease can progress in different
directions
High risk rate of sudden death
Disease progression with dyspnoe, chest
pains and syncope
Congestive heart disease with LV
remodelling
Atrium flutter with thromboembolia
31.
• Dyspnea, chest pain, dizziness, syncope usuallyare due to diastolic dysfunction. Systolic heart
function as a rule is normal
• Chest pain like in stenocardia as a rule develops
due to outflow obstruction and decreasing of
coronary circulation. Syncope as a rule appear
suddenly after emotional or physical strain due to
decreased outflow. Later syncope can appear at
rest
• Disease can manifest by arrhythmias ( atrium,
ventricular fluttering or fibrillation). Every
arrhythmia episode can be fatal for patient
32. Pathogenesis
• Ventricular septum hypertrophy so calleddisarray phenomenon of cell structure lead to
subsiding of myocardial tissue by connective
tissue and decreased pump function of heart and
form substrate for life threatening arrhythmias
• Outflow obstruction develops due to
disproportional ventricular septum hypertrophy
predispose to leaflets contact with septum and
produce increased gradient during systole.
• Prolonged hypertrophy predispose for disorder
of myocardium relaxation and development of
ventricular walls rigidity. Diastolic dysfunction
develops and later lead to systolyc heart
dysfunction.
33. Physical findings
• Appearance of patient is usual• Palpation: apex beat is wide and
dislocated to left. Ps is accelerated,
dicrotic.
• Auscultation- systolic murmur at apex
and in 4 left intercostal space near
sternum. Murmur is very variable. It can
be louder during physical exertion, in
vertical position, during tachycardia or
after nitrate or diuretic intake
34. Instrumental data
ECG
Chest X-ray examinig
Cholter ECG monitoring
Echo CG
Chest scanning
35. ECG data
Left ventricular hypertrophy signs
Negative T-waves in chest leads
Atypical deep Q-wave in II, III, aVF leads
Arrythmia and conductivity disorders (
atrium fibrillation, different blockages
• Cholter monitoring is helpful to reveal
threatening to life signs like unstable
ventricular tachycardia, atrium fibrillation,
signs of myocardium ischemia
36. Echo cardiography
• Ultrasound diagnostics is a gold standard ofHCMP confirmation
• Hypertrophy of ventricular septum and left
ventricular wall. Hypertrophy can be symmetric
and assymmetric (predominant septum
hypertrophy).
• Outflow obstruction with gradient more than 30
mmHg ( tests with physical strain)
• Dilation of left atrium, mitral regurgitation and in
terminal stages left ventricular dilation
37. Treatment
• Body weight decreasing• Exclude physical exertion
• Beta-adrenoblockers ( atenolol, carvedilol, nebivolol
etc) They decrease outflow obstruction at rest
• Verapamil decrease dyastolic dysfunction, can be
drug of choice in patients with bronchial asthma
• Anticoagulants ( varfarin, heparin, dipiridamol etc)
• Surgical treatment ( myoectomy by Morrow or
alcohol septum ablation) is necessary in refractory
medical treatment, progressive considerable
hypertrophy, gradient more than 50 mm Hg
• NB!
• Nitrates, ACEI medications, digoxin, nifedepin are
prohibited in obstructive cardiomyopathy
38. Dilative cardiomyopathy (DCMP)
• DCMP is primary myocardium disorderdue to different factors ( inheritance,
chronic viral myocarditis, immune
response disorders etc) and is characterised
by heart chambers dilation with left and
right ventricular systolic function disorder
and later diastolic dysfunction
39. DCMP classification
• Primary or idiopathic family CMP (genetic factorsautosome dominant type, simple DCMP with locuses1q32,2p31, 9q13, 10q21-q23; mitochondrial DCMP
are more frequent, connected with X-chromosome)
• Secondary CMP
Inflammatory (9%)
Ischemic (8%)
Due to hypertension
Due to amiloidosis
in AIDS patients
Chronic alcoholism
40.
Clinical presentation• Onset of disease has only few symptoms of
congestive heart disease. Disease progression
manifested by
• Dyspnea, asthmatic attacks
• Fatigability, muscle weakness
• Ventricular arrhythmia accompanied by syncope
• Atrium fibrillation, thromboembolia, systolic heart
dysfunction
• Right ventricular failure signs: edema of legs,
hepatomegaly, ascitis
41. Physical examining signs
• Appearance: acrocyanosis, extremities edema,orthopnoe position, neck veins swelling
• Auscultation: congestive moist rales in lungs apex
I sound is muffled, sometimes gallop rhythm or
additional III sound, systolic murmur of relative
mitral or tricuspid insufficiency, arrhythmia
• Chest palpation: enhanced, wide dislocated to left
and down apex beat
• Percussion: heart borders are dislocated to left
and right side
42. Instrumental data
• Chest X-ray Heart dilation-cardithoracic index ismore than 0,5, congestion in lungs or alveolar
edema
• ECG –nonspecific changes of ST segment and Twave, voltage decrease, QRS deformation, sinus
tachycardia, rhythm and conductivity disorders
• Echo- CG: dilation of chambers, systolic
dysfunction decreasing of LV output less than
55%, relative mitral and tricuspid regurgitation
• Endomyocardial biopsy in suspicion of
inflammatory CMP to evaluate myocardiocytes
distruction and inflammatory cells infiltration
43. Treatment
• Hospitalization• first signs of congestive heart disease to
specify its etiology;
• in cases of life threatening arrhythmias;
• progressive congestive heart disease:
• in acute conditions like heart asthma, lung
edema;
• complications like pneumonia, systemic
embolia, arrhythmia, syncope
44. Treatment
• Diet restriction of salt, water, coffee intake• Medications
• ACEI (enalapril, lisinopril, perindopril etc.) ( they
increase LV output, improve physical loading
tolerance, improve surviving of patients)
• Beta-adrenoblockers (atenolol, propranolol,
carvedilol, betacsolol etc)- they improve
hemodynamics, protect cardiomyocytes, decrease
tachycardia, prevent arrhythmias
• Treatment of different arrhythmia forms (amiadoron,
sotalol, antiarrhythmic medications class IA,
cardioversion)
• Surgical treatment heart transplantation
45. Questions
Prevention of non rheumatic carditis
Frequency and prognosis
Common clinical symptoms of myocarditis
Characteristic of main clinical variants
Additional (instrumental) methods of
invastigations
Medical check-up
Prevention of complications of NC.
Classification of heart failure
Principles of treatment of heart failure









































 Медицина
Медицина