Похожие презентации:
Polymyalgia rheumatica
1. Polymyalgia rheumatica
Dr Katya DolnikovD_katya@rambam.health.gov.il
2017
2. Introduction
• Polymyalgia rheumatica (PMR) is aninflammatory rheumatic condition
• Characterized clinically by :
– aching and morning stiffness in the shoulders, hip
girdle, and neck.
• It can be associated with giant cell (temporal)
arteritis (GCA), and the two disorders may
represent different manifestations of a shared
disease process
3.
4. Epidemiology
• Disease of adults over the age of 50, with a prevalence thatincreases progressively with advancing age
• The peak incidence of PMR occurs between ages 70 and 80
• PMR is relatively common. The lifetime risk of PMR is second only
to rheumatoid arthritis (RA) as a systemic rheumatic disease in
adults
• Women are affected two to three times more often than men
• Cases of familial aggregation are recognized
• The incidence is highest in Scandinavian countries and in people of
northern European descent
• PMR appears to be uncommon in Asian, African-American, and
Latino populations, though all racial and ethnic groups may be
affected.
5. Association with GCA
• PMR occurs in about 50% of patients withGCA
• The percentage of patients with PMR who
experience GCA at some point is ~10%
• The two disorders may not be active
synchronously
6. Pathogenesis
• The cause of polymyalgia rheumatica (PMR) isunknown
• Both environmental and genetic factors
appear to play a role
• Both PMR and GCA are associated with
specific alleles of human leukocyte antigen
(HLA)-DR4
• Some studies have suggested a cyclical pattern
in incidence and seasonal variation
7. Signs and Symptoms
• Aching and morning stiffness• Shoulders, hip girdle, neck, and torso are
involved
• Patients over the age of 50
• Symptoms are usually symmetric
• Recent, discrete change in musculoskeletal
symptoms
8.
9. Signs and Symptoms
• Morning stiffness > 30 minutes• Stiffness at the shoulders and hips may cause
trouble with dressing
• Stiffness may be so severe that there is difficulty
turning over in bed at night or arising from bed in
the morning.
• The ‘gel’ phenomenon, stiffness after inactivity, is
often notably severe in PMR
• An inability to actively abduct shoulders past 90
degrees because of stiffness is a typical finding
10. Signs and Symptoms
Shoulder pain is more common at presentation than hip pain
Pain is worse with movement and may interfere with sleep
Synovitis and bursitis - in peripheral joints, such as the knees, wrists, and MCPs
Synovitis and bursitis are thought to be the causes of the discomfort and stiffness
Swelling and tenosynovitis – Some patients develop swelling and pitting edema of
the hands, wrists, ankles, and top of the feet
Tenosynovitis can also cause carpal tunnel syndrome
Decreased range of motion – There may be decreased active and passive range of
motion of the shoulders, neck, and hips.
Muscle tenderness – not a prominent feature, and what tenderness there may be
about the shoulders is more likely due to synovial or bursal inflammation than
muscle involvement
Normal muscle strength
Systemic signs and symptoms – malaise, fatigue, depression, anorexia, weight loss,
and low-grade fever.
11. Laboratory findings
Elevated ESR, CRP (although can be normal)
Normocytic anemia
Thrombocytosis
Serologic tests, such as ANA, RF, ACPA are
typically negative
• Increase in liver enzymes, especially alkaline
phosphatase, although these abnormalities are
more common in patients with GCA than PMR
alone
12. Imaging
• Routine radiographs of inflamed joints do notshow abnormalities in patients with PMR
• MRI and US can demonstrate synovial
inflammation, with a predilection for extraarticular synovial structures (bursitis,
tenosynovitis)
• Synovitis is never erosive
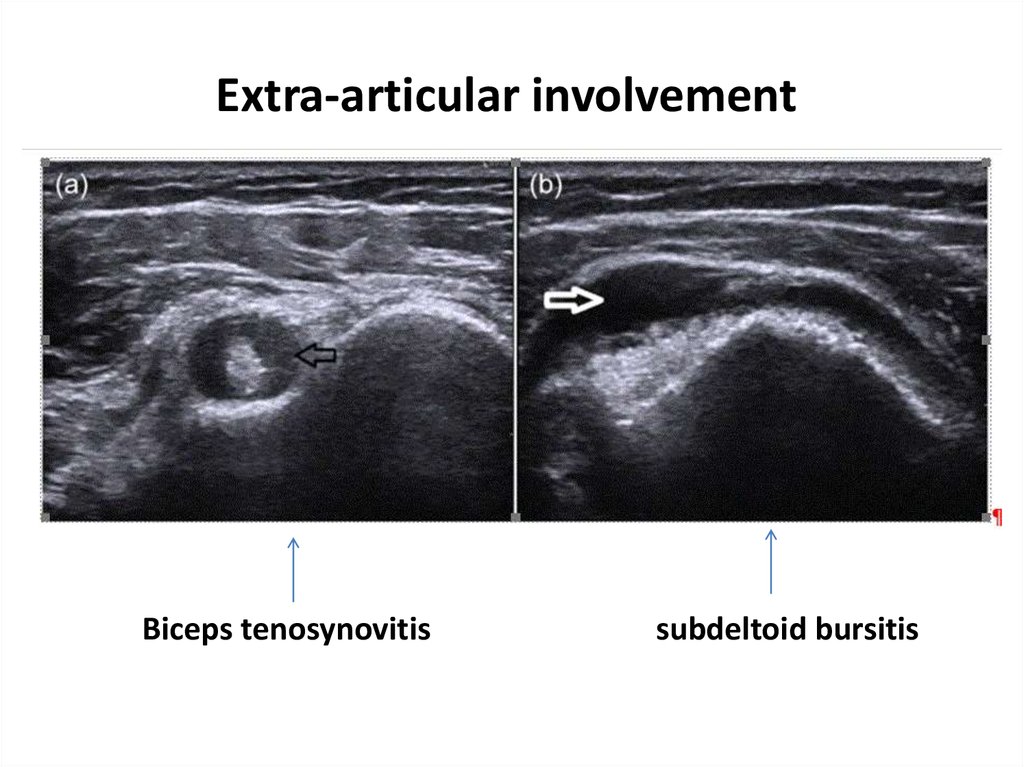
13. Extra-articular involvement
Biceps tenosynovitissubdeltoid bursitis
14. Evaluation of the patient
Medical history
Anemnesis
Physical examination
Assessment of the response to low-dose
glucocorticoids.
– Symptoms are generally 50 to 70 % better within 3 days of
prednisone (10 to 20 mg/day) and
– Almost all patients respond completely within two weeks
of initiation of therapy
• MRI or US may be helpful to assess whether there is
underlying bursitis or other evidence for inflammation
15. Diagnosis
• No pathognomonic test or established diagnosticcriteria for polymyalgia rheumatica (PMR)
• Presence of all of the following, after exclusion of
alternative disease:
– Age 50 years or older at disease onset
– Proximally and bilaterally distributed aching and morning
stiffness for at least two weeks
– 2/3 areas: neck or torso, shoulders or proximal regions of
the arms, and hips or proximal aspects of the thighs
– ESR ≥40 mm/h
– Rapid resolution of symptoms with low-dose
glucocorticoids.
16. Evaluation for GCA
• Patients with clinically "pure" PMR lack the classic findingsof GCA:
–
–
–
–
temporal artery tenderness,
headache,
jaw pain, visual symptoms
arm claudication.
• GCA may appear at any point during the clinical course of
PMR
• At every follow-up visit the patient should be monitored for
GCA signs and symptoms
• Evaluation, including biopsy, should be performed if
symptoms of GCA develop, even if patients are on
glucocorticoids
17. Diffrential Diagnosis
• Rheumatoid arthritis - symmetric polyarthritis of the small joints of thehands and feet, which is persistent and only partially responsive to low
doses of prednisone. In PMR fewer joints are swollen, and swelling
subsides completely in response to low-dose prednisone
• RS3PE syndrome - Remitting Seronegative Symmetrical Synovitis
with Pitting Edema, also described as the puffy edematous hand
syndrome or distal extremity swelling with pitting edema
• Inflammatory myopathy - Dermatomyositis or polymyositis present with
symmetric proximal muscle weakness
• Fibromyalgia
• Infective endocarditis
• Lyme disease may present with nonspecific constitutional symptoms that
include myalgias and arthralgias
• Malignancy
• Vasculitis
18. Treatment
• Practically all patients with PMR alone willrespond to 12.5 to 25 mg/day of prednisone
• Persistent aching and stiffness/ elevated CRP
or ESR under prednisone mandate pursuit of
an alternative diagnosis
• Slow tapering down
















 Медицина
Медицина