Похожие презентации:
Semey medical university siw age physiology of skeletal system in child
1. Semey medical university siw age physiology of skeletal system in child
SEMEY MEDICAL UNIVERSITYSIW
AGE PHYSIOLOGY OF SKELETAL
SYSTEM IN CHILD
SUBMITTED TO – OKSANA MAM
SUBMITTED BY – ABDULLAH
GROUP - 250
2. content
CONTENT3. Skeletal System
SKELETAL SYSTEM• Bones are made of several tissues
• Primarily made of collagen and hydroxyapatite - Ca10(PO4)6(OH)2
• About 206 bones in the human body
4. Functions of Skeletal System
FUNCTIONS OF SKELETAL SYSTEM• SUPPORT: Hard framework that supports and anchors the soft organs of the body.
• PROTECTION: Surrounds organs such as the brain and spinal cord.
• MOVEMENT: Allows for muscle attachment therefore the bones are used as levers.
• STORAGE: Minerals and lipids are stored within bone material.
• BLOOD CELL FORMATION: The bone marrow is responsible for blood cell production
5. Parts of the Skeletal System
PARTS OF THE SKELETAL SYSTEM• Axial skeleton
Skull and bones that support it
Includes vertebra and ribs
80 bones
• Appendicular skeleton
Limbs
126 bones
6. Features of a Long Bone
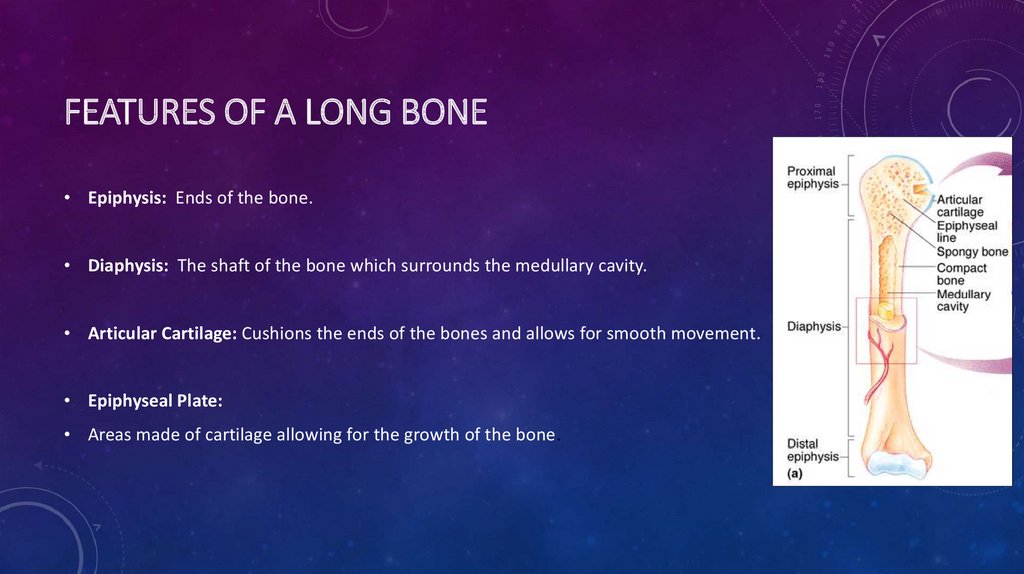
FEATURES OF A LONG BONE• Epiphysis: Ends of the bone.
• Diaphysis: The shaft of the bone which surrounds the medullary cavity.
• Articular Cartilage: Cushions the ends of the bones and allows for smooth movement.
• Epiphyseal Plate:
• Areas made of cartilage allowing for the growth of the bone.
7. Bone Development
BONE DEVELOPMENT• Initial skeleton of cartilage in infants
• Replaced with bone by osteoblasts
• More than 300 bones at birth – fuse to 206
• Always growing and breaking down
Osteoblasts – form new bone cells
Osteoclasts – break bone cells down
Osteocytes – mature bone cells
8. Bone Structure
BONE STRUCTURE• Periosteum – hard outer covering
• Cells for growth and repair
• Compact bone – hard strong layer
• Bone cells, blood vessels, protein with Ca and P
• Spongy bone – at ends of long bones
• Has small open spaces to lighten weight
• Marrow cavity – hollow in middle of long bones
9. Bone Marrow
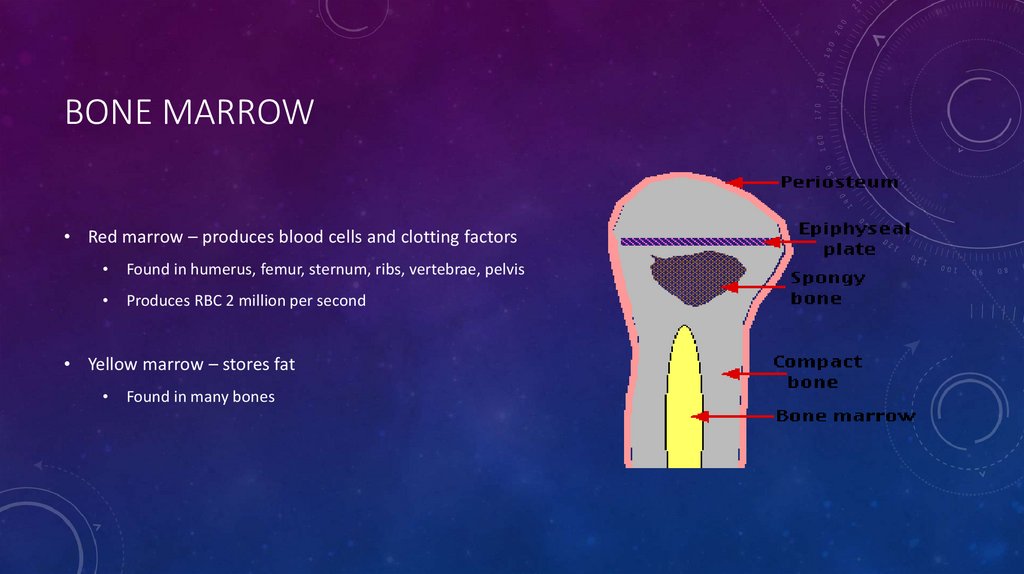
BONE MARROW• Red marrow – produces blood cells and clotting factors
Found in humerus, femur, sternum, ribs, vertebrae, pelvis
Produces RBC 2 million per second
• Yellow marrow – stores fat
Found in many bones
10. Skeletal system of child
SKELETAL SYSTEM OF CHILD• Bone in children and toddlers is more porous than adult bone, with wider haversian canals.
• A child's bones are more elastic than an adult's are. Two terms are important here: plasticity and
elasticity. Bones in children permit a greater degree of deformation before they break. At times, the
bone may deform but not fracture, a condition often described as a plastic deformation. At other times,
the bone may simply buckle to create what is described as a torus fracture. These patterns are not seen
in adults, in whom the bones' resistance and elasticity to angular deformation is significantly less
11.
• The periosteal sleeve is much thicker in children than in adults and acts as a restraint to displacement.Angular deformation of a child's bone may cause fracture of the cortices without displacement
("greenstick" fracture). The thick periosteal sleeve is important for pediatric skeletal remodeling.
Subperiosteal resection of a child's bone shows the regeneration potential associated with the
periosteum: the tubular bone eventually reforms inside the periosteal sleeve. Thus, the child's bone has
an innate potential to heal itself.
12.
• The epiphysis is an important part of the growing skeleton. It is a secondary ossification center. MercerRang emphasizes the importance of using accurate terminology in relation to these parts of the growing
skeleton. The physis is to the growth plate, which is a disklike structure at the end of the metaphysis;
the epiphysis is a cartilaginous structure that sits atop the physis.
13. Microscopic Anatomy
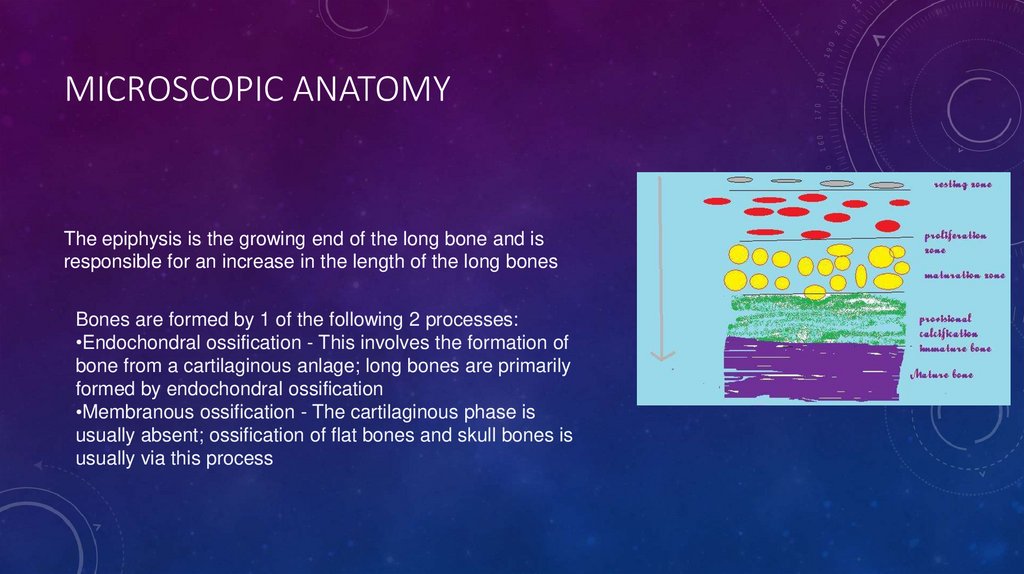
MICROSCOPIC ANATOMYThe epiphysis is the growing end of the long bone and is
responsible for an increase in the length of the long bones
Bones are formed by 1 of the following 2 processes:
•Endochondral ossification - This involves the formation of
bone from a cartilaginous anlage; long bones are primarily
formed by endochondral ossification
•Membranous ossification - The cartilaginous phase is
usually absent; ossification of flat bones and skull bones is
usually via this process
14.
• Histologically, the physis consists of a number of layers that reflect the process of bone formation. Thebasal layer consists of resting cartilage cells. These multiply under the influence of growth factors in the
zone of multiplication, and rounded cells are then seen. These rounded cells arrange themselves in
rows and mature in a loose cartilaginous matrix.
• Blood vessels from the metaphysis (see the image below) invade this zone to lay down minerals into the
matrix, and loose woven bone is then laid down in the zone of provisional calcification. Mature bone is
finally laid down in the metaphysis. A continuation of this process leads to an increase in the length of
the long bone.
15.
The epiphysis and the metaphysis are connected bymammillary processes internally and by the tough fibrous
periosteum externally, both of which resist displacement
forces. This attachment is not rigid and allows microscopic
translation forces, and this flexibility protects the structure
from injury.
Rang states that the epiphysis is periarticular and that
forces typically causing dislocation in the adult are likely to
cause epiphyseal or physeal injury in the child
16. Remodeling
REMODELING• Remodeling of a fracture or deformity is a process that is carried out more efficiently in the child than in
the adult. A deformity corrects itself by asymmetrical appositional formation of new bone. Remodeling
is influenced by a number of factors, including the following:
• Age - The younger the age, the better the remodeling potential
• Proximity to the physis - Fractures closer to the physis remodel better than those away from the physis
• Relation to the axis of joint motion - Deformities in the axis of joint motion remodel better than
deformities outside the axis of joint motion
• Rotational versus nonrotational deformity - Rotational deformities do not remodel and correct
themselves
17.
• An injury to a long bone can stimulate excessive growth and effectively create a temporary limb lengthdiscrepancy. The most common example is the stimulation of growth at the proximal femur after a
fracture in the shaft of the femur. This phenomenon allows the surgeon to accept some shortening in
the treatment of these fractures, given that they would be expected to correct with time.
• In contrast, a physeal injury can cause severe growth arrest and lead to limb length discrepancies and
deformities that can require years of treatment to correct. The most devastating of these injuries is
seen in the aftermath of pediatric infections. Septic arthritis of the hip leads to severe limb length
discrepancies and loss of function and stability.
18. Natural Variants
NATURAL VARIANTS• Bone in children undergoes serial changes and adaptations to achieve its adult form over a period of
years as the child reaches maturity.
• The secondary ossification centers appear at various ages; these can be a guide to bone age and true
skeletal age and thus are often helpful in resolving forensic and medicolegal issues. The fusion of these
secondary ossification centers also follows a set pattern, which is also useful in skeletal age
determination.
• For example, the ossification center of the greater trochanter appears at the age of 3 in girls and 6 in
boys, whereas that of the lesser trochanter appears at the age of 6 in both girls and boys. The
secondary ossification centers for the pubis appears at 9-11 years in girls and at 13-16 years in boys
19.
• At birth, the sutures in the skull are unfused at the anterior and posterior fontanelles. However, whereas theposterior fontanelle fuses soon after birth, the anterior fontanelle may not close until much later (eg, 12-18
months). Delayed closure of this fontanelle is seen in malnutrition and in rickets. Premature and rigid fusion of
skull bones is seen in craniosynostosis, which requires complex multidisciplinary procedures to correct.
• The alignment of the lower limbs also changes as the child progresses from crawling to the unsteady bipedal
gait of the toddler and, finally, to the established bipedal gait of the child.
• The toddler demonstrates a varus alignment at the knee and a waddle in the gait; the foot arches are yet not
developed. By about 2 years of age, knee alignment of the knee becomes neutral. Over the next few years,
knee alignment progresses to a physiologic genu valgum, which spontaneously corrects itself to a normal
tibiofemoral alignment by about 7 years of age. These variations are important to understand because parents
often consult an orthopedist for these issues, which require nothing more than careful clinical examination
and reassurance.
20.
• The varus and valgus alignments are believed to be dictated by the relative growth rates of the articularcartilage and the adjacent physeal zone. The physis grows almost 5 times faster than the articular
cartilage does. This difference may control varus and valgus alignment: varus develops if the medial
sides grow more slowly than the lateral sides, and valgus develops if they grow more quickly.
Gender and racial differences are well known. A number of studies have documented the evolution of
the tibiofemoral angle in children by using the tibiofemoral measurement and measurements of
intercondylar and intermalleolar distances. A study of European children showed that boys had a
greater tendency toward varus than girls did at the end of development, with lower intermalleolar and
intercondylar distances
21. defects
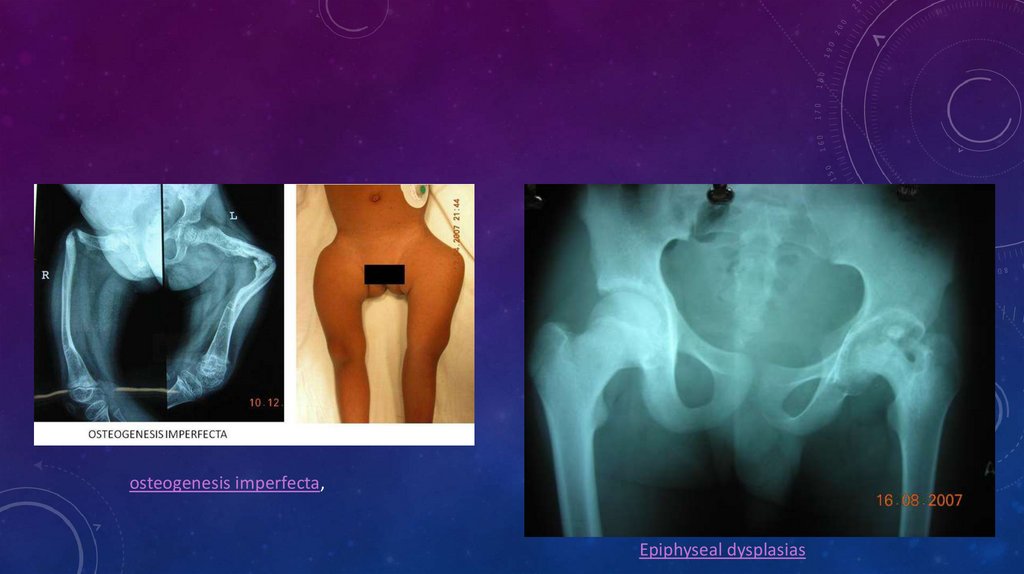
DEFECTS• Matrix deficiencies can give rise to a myriad of conditions, the best known of which is osteogenesis
imperfecta, which can lead to multiple pathologic fractures and deformities in childhood (see the image
below). Deficiencies of growth hormone and thyroid dysfunction also lead to stunting of growth and
dwarfism.
Infections and trauma can cause complete or partial physeal arrest, causing deformities and limb length
discrepancies (see the images below). Epiphyseal dysplasias also cause stunted growth and deformities
22.
osteogenesis imperfecta,Epiphyseal dysplasias
23. Broken Bones
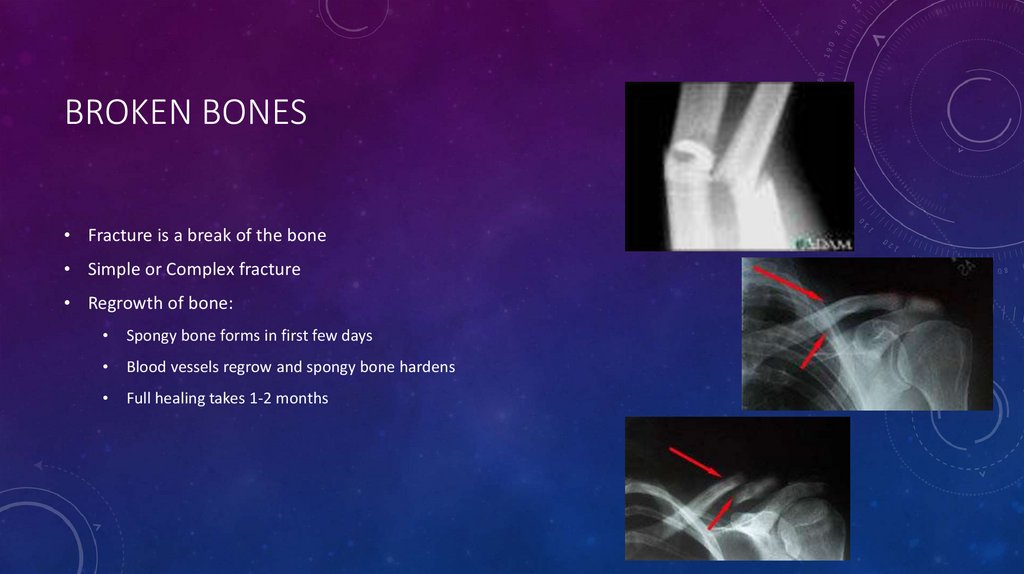
BROKEN BONES• Fracture is a break of the bone
• Simple or Complex fracture
• Regrowth of bone:
Spongy bone forms in first few days
Blood vessels regrow and spongy bone hardens
Full healing takes 1-2 months
24. refrence
REFRENCE• https://emedicine.medscape.com/article/1899256-overview#a4
• https://www.google.kz/search?q=skeletal+system+medscape&rlz=1C1ASRW_enKZ800KZ800&oq=skelet
al+system+medscape&aqs=chrome..69i57j69i60.9086j0j4&sourceid=chrome&ie=UTF-8
• Slide share
• Physiology essentials book
• http://www.innerbody.com/image/skelfov.html




















 Медицина
Медицина